Heel pain can stop you from walking comfortably, training properly, or even standing for long periods at work. Many people searching for answers about Heel Bursitis vs Plantar Fasciitis feel confused because both conditions affect the same region of the foot but cause pain in different ways. If you experience heel pain when walking or sharp discomfort first thing in the morning, understanding the difference between heel bursitis and plantar fasciitis symptoms can help you choose the right treatment early.
At Go Run Go Physio, we often assess patients who are unsure whether their pain sits at the back of the heel or under the foot. This guide explains the pain patterns, causes, diagnosis process, and physiotherapy options so you can take informed action.
Understanding Heel Pain and Why Location Matters
The heel contains several structures including the plantar fascia, Achilles tendon, bursae, fat pad and bone. When one of these tissues becomes irritated, you feel pain in a specific area.
Accurate location provides the first clue:
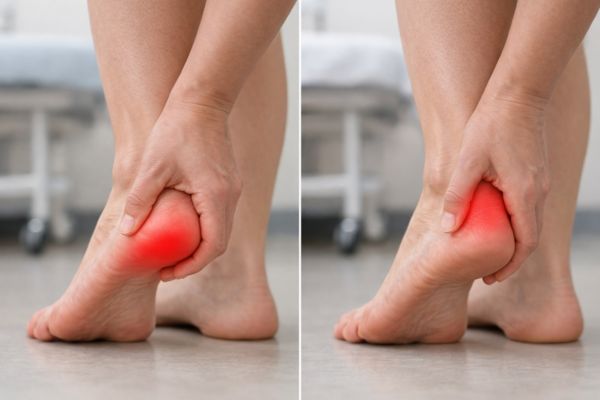
- Pain under the heel often relates to the plantar fascia
- Pain at the back of the heel may relate to the Achilles tendon or a bursa
- Swelling behind the heel can indicate bursitis
Patients often describe heel pain when walking as sharp with the first few steps, or dull and aching after long periods of standing. Identifying the exact spot of discomfort helps distinguish between Heel Bursitis vs Plantar Fasciitis.
Pain at Back of Heel vs Bottom of Heel
One of the simplest ways to understand the difference between heel bursitis and plantar fasciitis symptoms is to examine where the pain sits.
| Feature | Plantar Fasciitis | Heel Bursitis |
| Pain location | Bottom of heel, near arch | Back of heel, near Achilles |
| Morning pain | Common and intense | Less common |
| Swelling | Rare | Often present |
| Pain with tight shoes | Uncommon | Common |
| Tenderness to touch | Under heel | Behind heel |
If you feel pain at back of heel vs bottom of heel, this comparison can guide you, but clinical assessment remains important for confirmation.
Plantar Fasciitis and Its Common Features
Plantar fasciitis involves irritation of the thick band of tissue that runs from your heel bone to your toes. This structure supports your arch and absorbs shock during walking and running.
The most recognisable symptom is plantar fasciitis morning stiffness. Many patients report:
- Sharp pain during the first few steps after getting out of bed
- Pain after sitting for long periods
- Discomfort that eases with gentle movement
- Heel pain when walking long distances
Repeated strain, tight calf muscles, sudden increases in activity, and poor footwear can all contribute.
Runners, people who stand for extended hours, and those returning to activity after a break face higher risk.
Heel Bursitis and How It Develops
A bursa is a small fluid filled sac that reduces friction between tissues. At the heel, bursae sit near the Achilles tendon and the heel bone. When they become irritated, inflammation develops.
Heel bursitis typically causes:
- Pain at the back of the heel
- Visible swelling
- Redness or warmth in some cases
- Discomfort when wearing firm or tight shoes
- Pain when squeezing the back of the heel
Repetitive friction, sudden increase in running, poorly fitting footwear, and direct pressure on the heel often trigger heel bursitis.
Difference Between Heel Bursitis and Plantar Fasciitis Symptoms
Although both conditions involve the heel, their behaviour differs.
Plantar fasciitis morning stiffness remains one of the strongest indicators of plantar fascia irritation. Patients often describe improvement after a few minutes of walking.
Heel bursitis pain tends to feel more localised and may worsen with pressure from shoes. Swelling behind the heel provides a visual clue.
Another distinction relates to stretch tests. When a physiotherapist stretches the plantar fascia by lifting the toes upward, plantar fasciitis pain increases. When they compress the back of the heel, bursitis pain becomes more obvious.
Understanding the difference between heel bursitis and plantar fasciitis symptoms helps avoid delayed recovery caused by incorrect self-management.
Risk Factors and Common Triggers
Several factors contribute to heel pain conditions:
- Tight calf muscles
- Sudden increase in running volume
- Flat or high arched feet
- Prolonged standing
- Worn out footwear
- Reduced ankle mobility
Diagnosis and Clinical Assessment
A thorough assessment includes:
- Detailed history of pain onset
- Location mapping of symptoms
- Range of motion testing
- Strength testing of calf and foot muscles
- Gait analysis
Imaging such as ultrasound may help in persistent cases, but clinicians diagnose most cases clinically.
At Go Run Go Physio, assessment focuses on identifying movement faults, muscle imbalance and loading patterns rather than only treating symptoms.
Physiotherapy for Plantar Fasciitis and Heel Bursitis Treatment Physio
Effective physiotherapy for plantar fasciitis addresses both pain and the underlying mechanical drivers.
Management may include:
- Progressive calf strengthening
- Foot intrinsic muscle strengthening
- Load management advice
- Manual therapy
- Taping for short term support
- Footwear guidance
Patients with plantar fasciitis morning stiffness benefit from a graded loading programme rather than prolonged rest.
Heel bursitis treatment physio focuses on:
- Reducing compression at the back of the heel
- Modifying footwear
- Addressing Achilles tightness
- Controlled strengthening
- Activity modification
Rest alone rarely solves the issue. Targeted rehabilitation restores tissue tolerance and reduces recurrence.
Recovery Timelines and Expectations
Plantar fasciitis may improve within six to twelve weeks with consistent physiotherapy and load control. Chronic cases can take longer.
Heel bursitis often responds within several weeks once friction and pressure reduce, provided swelling settles and footwear changes occur.
Early intervention reduces long term disruption. Ignoring heel pain when walking often leads to compensatory patterns that strain other joints.
When to Seek Professional Care
Consider booking an assessment if:
- Pain persists longer than two weeks
- Swelling develops behind the heel
- Morning pain limits mobility
- Pain interferes with work or sport
- Self management has not improved symptoms
Go Run Go Physio provides individualised care plans designed around your activity goals.
Final Thoughts
Heel Bursitis vs Plantar Fasciitis can appear similar at first glance, yet their pain patterns, triggers and treatment plans differ. Identifying whether you have pain at back of heel vs bottom of heel provides the first step toward recovery. With accurate diagnosis and structured physiotherapy, most people return to normal activity without long term complications.
If you experience ongoing heel pain when walking or persistent plantar fasciitis morning stiffness, a personalised assessment at Go Run Go Physio can help you move comfortably again.
Frequently Asked Questions
Q1. What is the main difference between heel bursitis and plantar fasciitis?
Answer: The main difference lies in pain location. Plantar fasciitis causes pain under the heel with morning stiffness, while heel bursitis causes pain and swelling at the back of the heel.
Q2. Why do I feel heel pain when walking after rest?
Answer: This often indicates plantar fasciitis morning stiffness. The plantar fascia tightens during rest and becomes painful when stretched with the first steps.
Q3. Can heel bursitis cause pain at the bottom of the heel?
Answer: Heel bursitis usually causes pain at the back of the heel rather than underneath. Pain at the bottom more commonly suggests plantar fasciitis.
Q4. Is physiotherapy for plantar fasciitis effective?
Answer: Yes. Physiotherapy for plantar fasciitis focuses on progressive strengthening, load control, and movement correction. Most patients improve with structured rehabilitation.
Q5. How long does heel bursitis treatment physio take?
Answer: Mild cases may settle within a few weeks. More persistent cases can take longer depending on swelling and activity levels.